This post is for informational purposes only and should not be used in place of the advice of a medical professional.
As women age, their bodies go through significant changes that can affect gynecological health. To maintain good health during the senior years, it’s essential that senior women continue receiving gynecological care tailored to their specific needs. Gynecology for seniors encompasses a range of important health issues, from pelvic exams to the management of menopausal symptoms. Awareness and proactive management of these changes can lead to better overall health and quality of life.
Remember, maintaining a good health regime including lifestyle changes, staying informed about sexual health, and understanding the treatment options available to you are essential. Your healthcare provider can assist with health screenings and advice on managing chronic conditions that often affect senior women. Regular check-ups with a gynecologist or family medicine doctors familiar with your health conditions and gynecologic needs remain important, regardless of sexual activity or being past childbearing years.
Key Takeaways
- Gynecological health remains crucial for women as they age, with a focus on screening, symptom management, and maintaining quality of life.
- Preventive measures, screenings, and discussions on menopausal symptoms with a healthcare provider should be part of routine medical care for senior women.
- Treatment options for age-related gynecological issues should be tailored to each individual, considering their overall health and personal circumstances.
Video: Gynecology for Seniors
Understanding the Aging Process in Women
As women enter their senior years, their bodies experience significant changes, particularly in reproductive health and hormone balance, which can affect overall well-being.
Menopause and Hormonal Changes
Menopause marks the end of your menstrual periods and is a natural part of aging. This transition typically occurs between 45 and 55 years of age but can vary. Your body will produce less estrogen, leading to symptoms like hot flashes, night sweats, and vaginal dryness. These changes can start during the perimenopausal years, the time leading up to menopause. For those experiencing severe symptoms, treatments like hormone replacement therapy may offer relief. It’s also a time to discuss with your healthcare provider the potential benefits and risks of estrogen replacement therapy specific to your health conditions and family history.
Impact of Aging on Reproductive Health
The aging process significantly affects reproductive health in older women. Lower estrogen levels contribute to changes in the vaginal lining, which can lead to vaginal dryness and discomfort during sexual activity. It’s important to maintain regular gynecological exams, such as annual Pap smears and HPV tests, as the risk for conditions like cervical and uterine cancer increases with age.
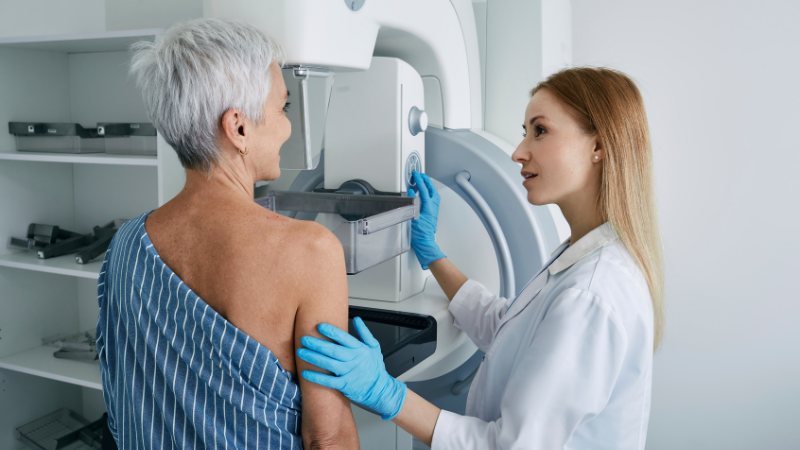
Breast exams and mammograms are crucial for early detection of breast cancer. Also, pelvic exams can help identify issues such as pelvic organ prolapse or urinary incontinence, common concerns for many senior women. Lastly, although less discussed, sexual health remains important, and you should feel comfortable addressing it with your healthcare provider.
Preventative Care
Your preventive healthcare should include discussions with your healthcare provider about screenings for cervical and breast cancer, managing common symptoms such as hot flashes and vaginal dryness, and understanding the risks and benefits of hormone replacement therapy. It’s also critical for older women to stay informed about their sexual health and treatment options for common conditions such as urinary incontinence and pelvic organ prolapse. Remember, your gynecological health remains a vital part of your well-being throughout your later years.
When considering gynecological care for senior women, pelvic exams and breast exams remain crucial, especially considering risks of cervical cancer, breast cancer, uterine cancer, and ovarian cancer. If you’re a woman in your senior years, you should be aware of the importance of these exams, as they play a role in early detection.
- Cervical Cancer Screening: After 65, many women may not require an annual pap smear if they’ve had normal screenings for the previous decade. However, your primary care physician may recommend continued testing if you have a family history or if you’ve had previous abnormal tests.
- Breast Health: Between mammograms and manual breast exams, screening should continue as breast cancer remains a risk. Discuss with your healthcare provider the frequency of these tests based on your medical history.
- Menopausal Symptoms: Issues like vaginal dryness, hot flashes, and night sweats can be common. Hormone replacement therapy may be an option for some, while others may benefit from non-hormonal treatment options.
- Vaginal and Urinary Tract Health: Vaginal discharge, urinary tract infections, and urinary incontinence can affect older women. Maintain regular visits to address these issues and learn about effective management strategies.
- Bone Health: Discuss bone density scans with your doctor, as your risk for osteoporosis increases with age.
- Monitoring chronic diseases like diabetes and high blood pressure becomes imperative. They can have an impact on your gynecological health and may lead to increased risk of heart disease or exacerbate menopausal symptoms. Regular blood tests and other assessments during your gynecology visits can help manage these chronic conditions effectively.
Common Gynecological Issues in Seniors
As women age, their bodies undergo various changes that can give rise to specific gynecological issues. Awareness and timely medical care can significantly improve the quality of life for senior women.
Urinary Tract Infections and Incontinence
Urinary tract infections (UTIs) are more prevalent in older women due to changes in the urinary system. A UTI can cause symptoms like a strong urge to urinate, pain during urination, and cloudy urine. Urinary incontinence, the involuntary leakage of urine, can also be a concern, often stemming from weakened pelvic floor muscles, and can significantly affect daily activities.
Strategies to manage these conditions include:
- Regular health screenings: A urine test can detect UTIs early, while bladder function tests can assess the cause of incontinence.
- Lifestyle changes: such as pelvic floor exercises, can strengthen muscles and improve bladder control.
Pelvic Pain and Prolapse
Pelvic pain in older women could signify a range of conditions. Pelvic organ prolapse, where the pelvic organs drop due to weakened muscles, can lead to a feeling of pressure or fullness in the pelvic area. This condition is closely associated with incontinence and bladder leakage.
Management may involve:
- Pelvic exams: Essential for evaluating pain and signs of prolapse.
- Treatment options: Ranging from lifestyle adjustments to surgical interventions for more severe cases of genital prolapse.
Vaginal Atrophy and Painful Sex
Vaginal atrophy occurs due to decreased estrogen levels, leading to thinning of vaginal walls and decreased vaginal lubrication, which can result in painful sexual intercourse. This is a common aspect of gynecological health affecting geriatric women.
Approaches to alleviating symptoms:
- Hormone replacement therapy (HRT): To help restore hormone levels and relieve symptoms.
- Estrogen replacement therapy: Applied topically to reduce discomfort and improve vaginal dryness.
It’s crucial for senior women to have an open dialogue with their healthcare provider about any signs of vulvovaginal inflammation, vaginal discharge, or pain during sexual activity as these may be indicative of underlying health concerns that require medical care. Regular gynecology visits and discussing treatment options can significantly contribute to maintaining good health in your later years.
Sexuality and Intimacy

As senior women navigate through their golden years, understanding the facets of sexuality and intimacy is crucial for maintaining a fulfilling quality of life. During this time, gynecological health becomes a vital component of overall health, influencing both physical and emotional well-being.
Sexual Activity in Older Age
You may wonder about the continuation of sexual activity as you age. It’s important to know that being sexually active is common among older adults, and you can maintain a satisfying sexual life well into your senior years. Vulvar and vaginal health are key to sexual function; however, changes like vaginal dryness or pelvic pain may affect your sexual experiences. These can be addressed with treatments such as vaginal lubrication or hormone replacement therapy. Regular gynecological care, including an annual exam and a pap test, ensures that you stay ahead of issues like vulvovaginal inflammation or more serious health conditions.
Addressing Sexual Dysfunction
If you face sexual dysfunction, it’s essential to consult with your healthcare provider. Senior women may experience a range of symptoms such as hot flashes and night sweats during menopause, which can impact sexual function. Discussing these symptoms with a primary care physician or an OB-GYN is a confident step toward finding effective treatment options.
Conditions like urinary incontinence and pelvic organ prolapse can also influence sexual health, and you might benefit from lifestyle changes, pelvic floor exercises, or medical intervention. Remember, maintaining good health through regular screenings and health screenings like blood pressure checks and blood tests is pivotal, as these can be independent risk factors for sexual dysfunction among older women.
Cancer Awareness and Management
Your health as a senior woman should include awareness and management strategies for cancers pertinent to your age group, such as cervical cancer, breast cancer, and uterine cancer. Regular screenings and understanding the symptoms are crucial for early detection and treatment.
Understanding Cervical and Breast Cancer
Cervical Cancer: Regular pelvic exams and Pap tests are important as they can detect precancerous conditions of the cervix. If you are over the age of 65 and have had normal Pap test results for several years, or if you have had your cervix removed (during a hysterectomy) for reasons not related to cancer, you may not need screening, but consult your doctor and follow his/her recommendation. However, if you’re still sexually active or have a history of cervical cancer or precancerous conditions, your doctor may advise continuing regular screenings.
- Key Screenings:
- Pap test: Should begin at age 21 and follow your healthcare provider’s guidelines for frequency.
- HPV test: Possible requirement, especially if you’ve had exposure to HPV, which is an independent risk factor for cervical cancer.
Breast Cancer: Mammograms should be a key part of your health care routine. Breast exams, either performed by your physician or through self-examinations, are also important for noticing any changes in your breast tissue.
- Risk Factors include:
- Age: The risk increases as you get older.
- Family history: If breast cancer is recurrent in your family, discuss the appropriate screening schedule with your healthcare provider.
- Hormone therapy: Especially estrogen replacement therapy, which can be associated with breast cancer development.
Uterine Cancer – Risks and Symptoms
Uterine cancer often presents symptoms such as vaginal bleeding after menopause or abnormal discharge. It’s essential to report these symptoms to your healthcare provider promptly for further investigation.
- Risk Factors:
- Age: It’s more common in women over 50 years of age.
- Endometrial hyperplasia: A condition characterized by thickening of the uterus lining, which can increase the risk of developing uterine cancer.
- Obesity: Being overweight can produce more estrogen, which can heighten the risk.
- Symptoms
- Postmenopausal bleeding
- Unusual vaginal discharge
- Pelvic pain
Treatment Options and Hormone Therapies
As you navigate the senior years of women’s health, understanding the various treatment options, particularly hormone therapies, is crucial. These therapies are tailored to alleviate symptoms associated with menopause, such as hot flashes and vaginal dryness, while also addressing long-term health concerns linked to decreased estrogen levels.
Hormone Replacement Therapy Pros and Cons
Hormone Replacement Therapy (HRT) caters to replenishing hormones, primarily estrogen, that are in lower quantities as you approach and enter menopause. HRT is highly effective in alleviating menopausal symptoms like hot flashes, night sweats, and vaginal dryness, and may also help in preventing osteoporosis.
- Pros:
- Alleviates menopausal symptoms
- May reduce the risk of osteoporosis and fractures
- Can improve vaginal health and alleviate urinary tract symptoms
- Cons:
- Increased risk for certain conditions, such as blood clots and breast cancer
- Risk of endometrial cancer if estrogen is taken without progesterone
- Potential side effects, including nausea and bloating
It’s essential that you discuss your personal and family history with your primary care physician or ob-gyn to weigh these factors, especially if you have a history of heart disease, breast cancer, or are at risk for gynecological cancers.
Alternatives to Traditional Hormone Therapy
For those for whom traditional HRT isn’t suitable or for senior women looking for other options, alternatives can help manage menopausal symptoms and maintain overall health.
- Lifestyle Changes: Implementation of dietary changes, regular exercise, and stress-reducing practices such as yoga can have a meaningful impact on symptoms.
- Non-Hormonal Medications: Treatments like low-dose antidepressants can mitigate hot flashes, while medications aimed at strengthening bone density can be a preventive measure against fractures.
- Vaginal Estrogen: To specifically target vaginal dryness and related discomfort, local estrogen treatments are available in the form of creams or rings.
Choosing the right treatment in your later years should be a collaborative process with your healthcare provider aimed at ensuring a healthy lifestyle and minimizing discomfort during menopause.
Navigating Healthcare
When it comes to gynecological care as you age, navigating the healthcare system effectively is essential for maintaining good health. It’s important to make informed choices about your healthcare providers and to understand the resources available to support you in managing your women’s health needs.
Choosing the Right Gynecologist
For senior women, choosing the right gynecologist or ob-gyn is a foundational step in healthcare. Your gynecologist should not only have expertise in senior health concerns such as menopausal symptoms, postmenopausal bleeding, and pelvic organ prolapse but also be someone with whom you are comfortable discussing sensitive information. Consider factors such as the doctor’s experience with senior women, their approach to treatment options, and how they involve you in decisions about your health.
- Look for a doctor who is board-certified and a member of credible organizations like the American College of Obstetricians and Gynecologists (ACOG).
- If you have a primary care physician, ask for referrals to reputable gynecologists who specialize in elderly women’s health.
- Before scheduling an appointment, confirm the gynecologist’s experience with health screenings relevant to your age group, like mammograms for breast cancer, pap tests, and HPV tests.
Patient Advocacy and Support Networks
Patient advocacy plays a critical role in ensuring that individual healthcare needs are met, especially for geriatric women managing chronic conditions or navigating complex health systems. Reliable support networks can also guide you through the process of finding appropriate healthcare providers, understanding your health conditions, and making lifestyle adjustments to manage symptoms like hot flashes or vaginal dryness.
- Utilize patient advocacy groups specifically focused on senior women’s health for resources and guidance.
- Online communities and local support groups can offer personal insights and recommendations for managing gynecological health in your later years.
- Maintain open communication with your healthcare provider about any healthcare concerns, including urinary tract infections, bladder control issues, and changes in your menstrual periods or vaginal discharge.
FAQs
As you navigate through your golden years, staying informed about gynecological health is crucial. This section answers common queries regarding gynecological care for senior women.
Is there a recommended age for women to cease gynecological examinations?
There is no set age for women to stop gynecological examinations, as individual health needs can vary. Women should discuss with their primary care physician or ob-gyn to make a personal decision based on their overall health, medical history, and family history. It’s important to continue these health visits, as they play a crucial role in the early detection and treatment of gynecological problems.
How often should senior women schedule gynecological exams?
Senior women should continue to have gynecological exams on a regular basis, at least annually unless advised otherwise by their healthcare provider. These exams are important for monitoring changes in the pelvic organs, screening for cervical cancer with a pap test, and evaluating any symptoms like pelvic pain or urinary incontinence.
How can seniors find a gynecologist specializing in geriatric care?
Ask for referrals from primary care physicians, check with local healthcare networks, and ensure the selected gynecologist has experience in geriatric gynecology.
Additional Reading
Conclusion
In your senior years, maintaining good health becomes paramount, and gynecological care is no exception. Regular health screenings, including a pelvic exam and a breast exam, are vital for early detection of conditions like cervical cancer and breast cancer. Although menstrual periods have ceased, you should remain vigilant about any postmenopausal bleeding, as it could indicate serious health issues such as uterine cancer or ovarian cancer.
A gynecological exam should continue to take place on a regular basis. Senior women often experience menopausal symptoms like hot flashes and vaginal dryness. Your healthcare provider can discuss treatment options, which might include hormone replacement therapy. Additionally, issues like urinary incontinence or pelvic organ prolapse need to be monitored, as they can affect your quality of life in the later years.
Your primary care physician or ob-gyn can help you manage gynecologic needs, tailoring care to any family history of chronic diseases or individual health conditions. Remember, an annual visit is not only about reproductive health; it’s a comprehensive review of your overall health—from blood pressure checks to bladder function assessments.
In summary, don’t overlook the importance of annual exams and foster a proactive relationship with your medical care team to navigate your golden years with confidence.
Have you found going for gynecological exams helpful in managing your healthcare? Please comment below.










I am 71years old and it has been a while since I have seen a gynocologist. I am having some female health issues and would like to see a female gynocologist in the Flowood area, if possible.
Can you help me or put me in touch with someone who can? Thank you in advance for your help?
Hello Judy,
Thank you for visiting LivingYourSeniorLife and taking the time to reach out.I understand the importance of finding the right healthcare provider, especially when it comes to sensitive matters like female health issues.
While I’m not personally able to refer you to specific healthcare providers, I can certainly offer some guidance on how to find a female gynecologist in the Flowood area. One option is to reach out to your primary care physician for recommendations. They often have networks of specialists they can refer you to.
Additionally, you can utilize online resources such as healthcare provider directories or websites like Healthgrades or Zocdoc. These platforms allow you to search for gynecologists in your area and filter by gender preferences.
Another avenue is to contact local hospitals or women’s health clinics in the Flowood area. They may be able to provide you with a list of female gynecologists who are accepting new patients.
I hope these suggestions are helpful to you in your search for a healthcare provider. If you have any further questions or need assistance, please don’t hesitate to reach out.
Wishing you the best of health,
Debbie