If you have ever wondered about the relationship between arthritis and rheumatism, you are not alone. These terms are often used interchangeably, but are they actually the same thing? The purpose of this article, About Arthritis and Rheumatism, is to provide you with answers. You will learn about these conditions, how they are related, their symptoms, causes, and treatments.
It is important to note that this article is for informational purposes only. It should not be used as a substitute for medical advice or consultation with a healthcare professional. With that said, let’s dive into the world of arthritis and rheumatism.
Key Takeaways:
- Arthritis and rheumatism are two different conditions that affect the joints and cause pain and inflammation. Here are some key takeaways to keep in mind:
- Arthritis is a general term that refers to joint inflammation, while rheumatism is a non-specific term that is often used to describe joint and muscle pain.
- Rheumatoid arthritis is a chronic autoimmune disorder that mainly affects the joints and can lead to joint destruction if left untreated. The exact cause of RA is uncertain, but genetic and environmental factors, such as family history and smoking, contribute to its development.
- Osteoarthritis is the most common type of arthritis, which occurs when the protective cartilage that cushions the ends of your bones wears down over time.
- Symptoms of arthritis include joint pain, stiffness, swelling, and loss of mobility. These symptoms can worsen over time if left untreated.
- Treatment for arthritis and rheumatism may include medication, physical therapy, lifestyle changes, and surgery in severe cases.
- It is important to see a healthcare provider if you are experiencing joint pain or other symptoms of arthritis or rheumatism. They can diagnose your condition and develop a personalized treatment plan to help manage your symptoms and improve your quality of life.
What Is Arthritis?
Arthritis is a term used to describe a group of conditions that cause inflammation in one or more joints. It can be thought of as an umbrella term for over 100 different types of arthritis, each with its own unique characteristics. Two common types of arthritis are osteoarthritis, also known as degenerative arthritis, and rheumatoid arthritis, often referred to as inflammatory arthritis.
Arthritis occurs when the body experiences inflammation in one or more of the joints. This inflammation causes pain, stiffness and also can limit the range of motion. The pain that is experienced can range from mild to chronic and may subside only to come back.
Symptoms of arthritis include joint pain, stiffness, and limited range of motion. These symptoms can range from mild to chronic and may come and go. Arthritis can affect various joints in the body, including the knees, hands, wrists, shoulders, ankles, hips, and small joints in the fingers and toes. It can also affect other parts of the body, including bones, muscles, tendons, ligaments, and cartilage.
Arthritis can be caused by a variety of factors, including genetics, injury, infection, and autoimmune disorders such as lupus, psoriasis, and juvenile idiopathic arthritis. Other types of arthritis include gout, reactive arthritis, psoriatic arthritis, and carpal tunnel syndrome.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is a chronic inflammatory disorder that affects the joints, causing pain, swelling, and stiffness. It is an autoimmune disease in which the immune system mistakenly attacks the body’s own tissues, including those of the joints. This can lead to bone erosion and joint deformity over time. RA is a progressive disease that can also damage internal organs, eyes, lungs, heart, and other body parts.
Rheumatoid arthritis can affect people of all ages, but it is most commonly diagnosed between the ages of 40 and 60. According to a study, more than 50 million adults and 300,000 children in the United States have arthritis. It is more common in women and is seen more often as people age.
Symptoms of RA include joint pain, tenderness, swelling, and stiffness that lasts for six weeks or longer. Morning stiffness that lasts for 30 minutes or longer is also a common symptom. RA commonly affects joints in the hands, wrists, and knees, and usually appears symmetrically on both sides of the body. Some people with RA may also develop fleshy lumps called rheumatoid nodules, which form under the skin around the affected joints.
Video: About Arthritis and Rheumatism
Symptoms of Rheumatoid Arthritis
If you have Rheumatoid Arthritis (RA), you may experience:
- Tender, warm, swollen joints
- Joint Inflammation
- Joint Stiffness – especially in the morning and after inactivity.
- Fatigue
- Fever
- Loss of appetite
Causes of Rheumatoid Arthritis

It is thought that Rheumatism is caused by a combination of environmental and genetic factors, as was studied by Smolen, J. S., Aletaha, D., and McInnes, I. B at the University of Glasgow in 2016.
Research suggests that a family history of rheumatoid arthritis increases the risk of developing the condition by 3-5 times.
Environmental factors, such as smoking, are also thought to increase the risk of developing rheumatoid arthritis, particularly in Caucasians. Though not fully understood, an increased risk of developing rheumatoid arthritis is thought to be correlated to exposure to asbestos or silica.
While the exact causes of rheumatoid arthritis are not fully understood, it is considered an autoimmune disorder where the immune system mistakenly attacks the body’s own tissues, including the joints, organs, lungs, heart, blood vessels, and nerves.
Diagnosis of Rheumatoid Arthritis

Diagnosing Rheumatoid Arthritis can be challenging, especially in the early stages, as symptoms may mimic those of other diseases such as lupus or fibromyalgia. Therefore, it is important to consult a rheumatologist, a doctor who specializes in diagnosing and treating rheumatic diseases, if you suspect that you have Rheumatoid Arthritis.
If you suspect that you have Rheumatoid Arthritis, the first step is to make an appointment with your doctor. During your appointment, your doctor will ask you questions about your symptoms, such as when you first started experiencing them, how often they occur, and how severe they are.
After discussing your symptoms, your doctor will perform a physical examination and check for warmth, swelling, and redness in the affected joints. To confirm the diagnosis, your doctor may order blood tests to check for inflammation levels and the presence of rheumatoid factor.
Imaging tests, such as X-rays, MRIs, or ultrasounds, may also be ordered to assess the severity of the disease and track its progression. X-rays can show signs of osteopenia, soft tissue swelling, and decreased joint space. An MRI or ultrasound can provide more detailed images of the joints and surrounding tissues.
Treatment of Rheumatoid Arthritis
If you have Rheumatoid Arthritis, you may be wondering what treatment options are available to you. While there is no cure for the disease, there are treatments that can help manage the symptoms, slow down the progression, and lessen the pain. In this section, we will discuss some of the most common treatments for Rheumatoid Arthritis.
Medication

Medication is one of the most common treatments for Rheumatoid Arthritis.
Disease-modifying anti-rheumatic drugs
Disease-modifying anti-rheumatic drugs (DMARDs) are a type of medication that should be started early in treatment. They have been found to improve symptoms, decrease joint damage, and improve overall functional abilities.
Some common anti-rheumatic drugs include:
- Methotrexate
- Hydroxychloroquine
- Sulfasalazine
- Leflunomide
- Rituximab and tocilizumab are monoclonal antibodies and are also DMARDs
Methotrexate is the most commonly used drug and is often the first one prescribed. It can also be used with other anti-rheumatic drugs to increase remission rates. After six months, 21% more people had an improvement in their symptoms using a combination of rituximab and methotrexate than those that didn’t.
Anti-inflammatory Drugs
NSAIDs
Anti-inflammatory drugs, such as Nonsteroidal anti-inflammatory drugs (NSAIDs), have been found to reduce both pain and stiffness in those suffering from RA. However, because they do not affect the underlying disease, they are usually not the first choice. Also, those with gastrointestinal, cardiovascular, or kidney-related issues should use caution with taking NSAIDs. Stomach irritation, heart problems, and kidney damage are possible side effects of NSAIDs.
Examples of NSAID drugs include:
- Aspirin
- Celebrex
- Diclofenac
- Diflunisal
- Etodolac
- Ibuprofen (Motrin, Advil)
- indomethacin
Non-NSAID
Non-NSAID drugs to relieve pain, like paracetamol, may help reduce the pain; however, like NSAIDs, they do not change the underlying disease.
Examples of Non-NSAID drugs
- Acetaminophen (Tylenol)
- Naproxen (Aleve)
- Paracetamol – may be associated with an increased risk of developing ulcers.
- Tramadol
Physiotherapy/Physical Therapy
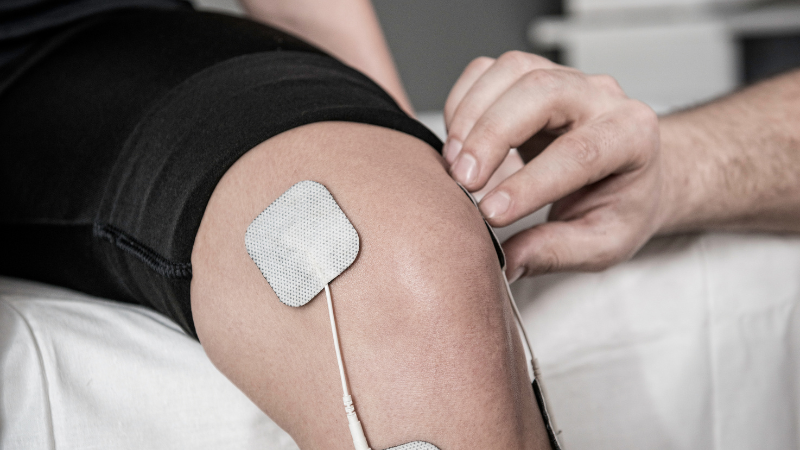
Physiotherapy and physical therapy can help alleviate the soreness of muscles and reduce inflammation. Applying heat and cold may also help.
Electrical stimulation, the elicitation of muscle contraction using electric impulses, can also be used in conjunction with physical therapy. A TENS unit is a small device that sends electrical signals into your body through electrodes placed on your skin near the area that hurts. Though some people find relief with Electrical stimulation, it is usually short-lived.
Lifestyle
Diet
Though there isn’t a particular diet for those dealing with Rheumatoid Arthritis, there are foods with an anti-inflammatory effect.
Some of these anti-inflammatory foods include:
- Coldwater fish – Salmon, tuna, sardines, herring
- Olive oil
- Fruits
- Vegetables
- Nuts/Seeds
- Beans
- Green Tea
Foods to Avoid:
- Beef
- Dairy
- Corn Oil
- Fried Food, Fast Food, and Processed Foods
- Salt
- Sugar
- Alcohol
Supplements
Supplements are in abundance, so it’s important to talk with your healthcare provider before adding supplements to your routine. Some supplements can interact with other medications, so it’s best to err on the safe side. But what are some supplements that are said to help with inflammation?
Fish Oil
Contains Omega-3 fatty acids, which are thought to have anti-inflammatory properties. However, be aware that the cold-water fish, such as salmon and tuna, that fish oil is derived from can contain high mercury levels, so do your research.
Fish Oil can also slow blood clotting, so you will want to talk to your doctor, especially if you take blood thinners or high blood pressure medications.
Turmeric
A spice that contains a compound, curcumin, which has anti-inflammatory properties. A small study published in the Journal of Medicinal Food concluded that turmeric and its compounds could help alleviate pain and inflammation. Being that this was a small study, though, more research needs to be done to see if the results translate into a more extensive study population.
Like Fish Oil, turmeric can slow blood clotting, so be sure to consult with your health care provider.
Boswellia or Indian Frankincense
Has potent anti-inflammatory and analgesic properties. Like other supplement studies, more research needs to be conducted, but according to arthritis.org, Boswellia does look promising in treating rheumatoid arthritis.
Exercise

Making lifestyle changes can also help manage the symptoms of Rheumatoid Arthritis. Rest is important, but so is exercise. Walking is one of the best exercises you can do. It is low-impact and helps to maintain muscle strength and physical function. Exercise can also combat fatigue.
You’ll want to start with gentle exercise that does not lead to more inflammation. As always, before beginning any exercise program, consult with your doctor.
Compression Gloves
Numerous companies make compression gloves for arthritic hands, many with great reviews. Compression gloves can help alleviate arthritis pain and discomfort.
May be of Reading Interest: 3 Best Gloves For Arthritis in Hands
Support

Living with rheumatoid arthritis can be challenging, but you don’t have to go through it alone. Consider joining a local support group or online community through the Arthritis Foundation. Connecting with others who understand what you’re going through can improve your quality of life and reduce feelings of depression and disability. Visit www.arthritis.org to find a local group or explore their online resources.
FAQs
What are the signs that rheumatoid arthritis is progressing?
Rheumatoid arthritis is a chronic autoimmune disease that can cause inflammation and damage to the joints and other organs in the body. As the disease progresses, you may experience increased joint pain, stiffness, and swelling. You may also notice a decreased range of motion and difficulty with daily activities such as dressing, grooming, and walking. In some cases, rheumatoid arthritis can also cause fatigue, fever, and weight loss.
What are seven signs of rheumatoid arthritis?

The seven signs of rheumatoid arthritis, as identified by the Arthritis Foundation, are:
Joint Pain, Swelling, and Stiffness
Fatigue and Weakness
Loss of Appetite and Weight Loss
Low-grade Fever
Dry Eyes and Mouth
Nodules Under the Skin
Joint Deformity and Loss of Function
Additional Reading
Conclusion
In conclusion, having a better understanding of rheumatoid arthritis can help you manage the disease more effectively. By recognizing the symptoms you are experiencing, you can address them individually and work with your doctor to develop a personalized treatment plan that suits your needs.
It is important to remember that what works for someone else may not necessarily work for you, so it’s essential to remain open to different treatments and approaches. Don’t be afraid to ask questions or seek support from others who are going through similar experiences. Remember, managing rheumatoid arthritis is a journey, and with the right knowledge, resources, and support, you can successfully navigate it and live a fulfilling life.
I hope in reading, About Arthritis and Rheumatism, some of your questions have been answered. What’s important is that you discuss your symptoms with your doctor and make a treatment plan that is beneficial to you.
Have you experienced arthritis or any treatments; do you have any questions or comments? Please comment below – I would love to hear from you.